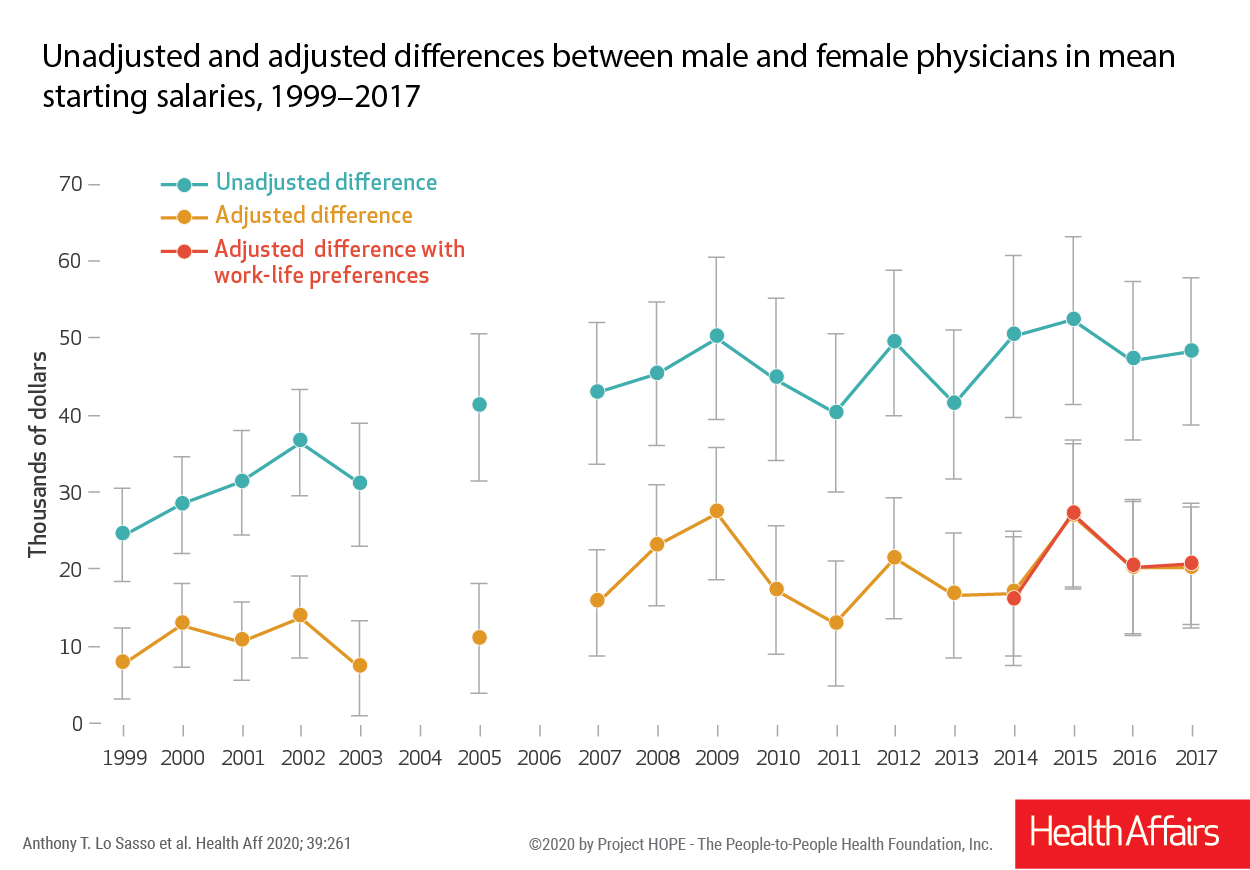
 Researchers looked at survey data from new physicians in New York who accepted positions in patient care from 1999-2017 to examine how the gender gap in total starting pay evolved and the extent to which preferences in work-life balance factors affect the gap. Their findings appear in a new study, “Differences in starting pay for male and female physicians persist; Explanations for the gender gap remain elusive,” in Health Affairs. (Photo courtesy of Health Affairs)
Researchers looked at survey data from new physicians in New York who accepted positions in patient care from 1999-2017 to examine how the gender gap in total starting pay evolved and the extent to which preferences in work-life balance factors affect the gap. Their findings appear in a new study, “Differences in starting pay for male and female physicians persist; Explanations for the gender gap remain elusive,” in Health Affairs. (Photo courtesy of Health Affairs)CHICAGO — When taking into account factors such as work-life balance, the pay difference between new male and female physicians is still largely unaccounted for, according to findings that were published Jan. 22 ahead of print and will also appear in the February issue of the journal Health Affairs.
The new study, “Differences in starting pay for male and female physicians persist; Explanations for the gender gap remain elusive,” highlights continued disparity and persistent unexplained gender differences in pay for new physicians. Researchers looked at survey data from new physicians in New York who accepted positions in patient care from 1999-2017, and examined how the gender gap in total starting pay evolved and the extent to which preferences in work-life balance factors affect the gap.
“Prior research, including my own, has documented a large gender gap in salary even after accounting for medical specialty, hours seeing patients, and practice setting among other factors. But we’re first to incorporate physician preferences for work-life balance factors,” said lead author Anthony T. Lo Sasso, a professor of economics in DePaul University’s Driehaus College of Business.
Specialty chosen consistently explained 40-55% of the total starting salary differences, while differences in number of job offers explained 2-9%, and hours of time spent in patient care explained 7%, according to the findings. However, despite women being much more likely than men to report that work-life balance factors were “very important”, when these work-life balance variables were added to the researchers’ model, the salary differences changed only negligibly (less than $1,000). In addition, work-life balance factors when added in from 2014-17, only explained less than 1% of the starting salary difference. Overall, 30-39% of the starting salary difference remains unexplained, the research showed.
Co-authors of the study are David Armstrong and Gaetano Forte from the Center for Health Workforce Studies at the University of Albany, and Susan E. Gerber, a faculty member in the departments of obstetrics and gynecology and medical education housed in the Feinberg School of Medicine at Northwestern University.
Among the findings:
- A pay average difference of almost $37,000 ($235,044 for men, $198,426 for women) over the entire period of the study, but a pay average difference of almost $49,000 ($271,267 for men, $222,268 for women) for the more recent 2014-17 period.
- Even after accounting for observed differences in specialty and other factors, the pay gap grew over the nearly 20-year period, from $7,700 in 1999 to $20,200 in 2017.
The research also showed that women:
- Chose primary care fields more often and surgical specialties less often than men (36.7% vs. 30.8%).
- Less commonly reported spending 50 hours or more per week in direct patient care relative to men (22.7% vs. 34.7%).
- Had six or more job offers less often than men (11.1% vs. 18.4%).
- From 2014-17, were consistently more likely to rate control over each measure of work-life balance preference as “very important” in comparison to men (42-56% vs. 33-45% depending on question).
As next steps, researchers may include a series of questions in future surveys of new physicians that get at non-monetary job characteristics and whether their new job has those characteristics, which could help account for differences in the job beyond salary, explained Lo Sasso.
“To continue searching for an answer to this question, we believe it’s important to dive deeper into job characteristics that are important and could plausibly differ by gender such as the role of negotiation, the amount of call, and the predictability of hours, among other factors,” said Lo Sasso. “I’m primarily a quantitative researcher, but I’m not adverse to doing some qualitative research and talking to new physicians to learn about their job search experience.
“Until a firm conclusion has been reached on the reasons behind the gender pay gap in new physicians, it’s important for employers to remain vigilant in ensuring pay equity. Greater transparency is needed, such as the salary difference between those physicians willing to do more on-call work and those who aren’t. We also encourage residency programs to provide increased training on job-searching skills such as salary negotiation,” Lo Sasso added.
###
Source:
Anthony Lo Sasso
312-362-1242
Media contact:
Russell Dorn
312-362-7128